THE TECHNOLOGICAL FIGHT AGAINST THE SILENT THIEF OF SIGHT
With 12% of new cases of registered blindness each year due to glaucoma, and 80 million people living with glaucoma - expected to rise to 112 million by 2040 - it is heartening to know that advances in optical coherence tomography (OCT) technology, new treatments and innovative research are contributing to earlier detection. This is set to ensure treatment at the right time and better patient outcomes.
The upward trend of this silent stealer of sight, delays in starting treatment, and poor patient adherence, is causing alarm, as Professor Dr Christian Mardin, Consultant Ophthalmologist in Erlangen-Nurnberg, Germany, explained –
“Lack of awareness causes permanent vision loss, with a progressive loss of visual field. Early glaucoma has no symptoms. Every person over 40 should go to their optometrist or ophthalmologist to get their optic nerve head checked. It ties in very well with buying their first pair of reading glasses.”
The benefits of a non-invasive, OCT scan can reveal the first signs, perhaps years before symptoms become apparent. There can be up to 40% damage to the optic nerve before any visual changes are noticed - this vision loss cannot be restored. This damage can lead to problems with peripheral and tunnel vision, narrowing of the field of vision and general loss of visual acuity or contrast perception.
Risk factors for glaucoma include:
- Age over 40
- A family history of glaucoma
- Shortsightedness
- Diabetes
- African-Caribbean origin
Professor Mardin explained –
“Myopia, along with other comorbidities, makes diagnosis more difficult. You are up to three times more likely to develop glaucoma if you are myopic, but now we can pick up these symptoms very early and treatment can begin.”
A global multi-center research project focused on the phenotyping of myopic and glaucomatous eyes holds out hope for earlier detection in patients with these co-existing conditions. The Glaucoma Myopia OCT Phenotyping Consortium brings together specialists from 13 clinical centers and seven countries, including the University Hospital Erlangen, who are collecting a unique data set which will facilitate research ultimately improving outcomes for this patient group.
“Some conditions masquerade and mimic the symptoms of glaucoma but now, with advances in OCT, mean we can make fast and meaningful measurements of the optic nerve head, and by freezing the image we can improve the quality of the baseline and reproducibility of the follow-up scans. In glaucoma treatment time and speed are essential.”
MASQUERADERS
In addition to patients with high myopia, patients with diabetes, kidney disease and hypertension can frequently have glaucoma as a co-existing condition, particularly when they are elderly, but there is so much more to this picture, as Sanjay Asrani, Professor of Ophthalmology at Duke Eye Center, North Carolina, USA explained –
“I have chanced upon signs which masquerade as glaucoma on an OCT scan. Branch retinal artery occlusions or coton wool spots – small infarcts or blood vessel closures - can result in an initial swelling in the nerve fibre layer. They are transient and disappear in a few weeks and are often caused by high blood pressure or kidney disease."
“The resultant thinning of the tissues can resemble glaucoma, with a loss of peripheral vision. In 99% of cases we are not lucky enough to visualise the events while they are happening, so no one knows the frequency of how often they occur,” said Dr Asrani.
With a few cases of masquerading identified each month in the Duke Eye Center clinic, there is strong evidence to suggest that this is happening in every eye clinic with the possibility of unnecessary treatment being initiated. Clinicians should always consider the distinct possibility that thinning revealed by the OCT may be due to these conditions.
“There are downsides to unnecessary treatment - psychological, economical and even the risk of unnecessary sight loss if more aggressive treatments are used.”
The use of AI is expected to combat the issues of over and under treating glaucoma patients in what are often very busy clinics. The rise of telemedicine – boosted by home monitoring apps which were accelerated during Covid – are also expected to improve treatment plans for many patients in remote areas or with disabilities. This is also expected to reduce waiting times for those who need to be seen by a clinician.
Dr Asrani’s 30-year career in the field of glaucoma care has seen great advances in early diagnosis, largely thanks to enhancements in OCT imaging –
“We are catching patients younger and earlier with beter screening techniques using both anterior and posterior segment OCT imaging.”
Ten years on SPECTRALIS GMPE – Glaucoma Module Premium Edition – continues to provide a tangible benchmark in clinical routine, believes Dr Asrani –
“I began using it at the outset. It gave us the ability to standardise measurements, thanks to the strict protocols and consideration of three key elements -
*Ganglion cells
*Nerve fiber tissue
*CuppingThe all-in-one software programme, rather than three different elements which we need to draw together, GMPE, has helped us to identify masqueraders that we might not have picked up before. The absence of cupping in the presence of nerve fibre layer and ganglion cell loss gives us clues that the change may not be due to glaucoma but rather due to hypertension.”
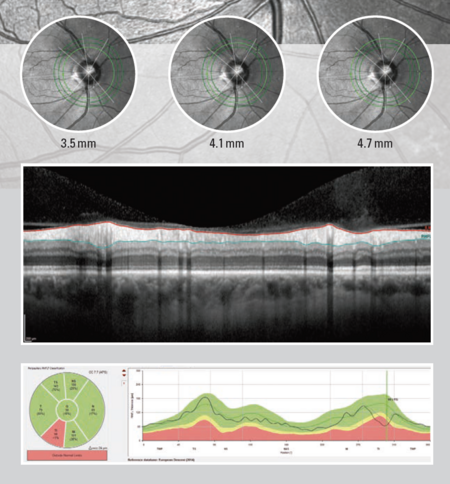
The SPECTRALIS GMPE Anatomic Positioning System (APS) uses two fixed anatomic landmarks of the center of Bruch’s membrane opening and the fovea of each eye, ensuring accurate comparison and characteristisation of fine structures relevant in glaucoma diagnostics. The precision of the SPECTRALIS AutoRescan function allows confident identification and monitoring of structural changes from one visit to the next because the same location for comparison is guaranteed due to APS. As a progressive disease, reliably detecting as small as one microns of change is vital to clinicians who trust that OCT imaging provides objective, quantitative, results.
Clinicians believe that using advanced OCT modalities is an ethical obligation to find and track disease, and to identify changes before vision loss occurs.
Optimistic about the future care of patients, Dr Asrani said that a glaucoma diagnosis can cause fear of vision loss, which is why many avoid thinking about it unless they are encouraged by their family -
“We expect to see glaucoma occurring in 60-70% of first-degree relatives, and between 30-40% of cases when a grandparent has had glaucoma, but the next few years is set to see even greater treatment options, which are simpler and safer, so early detection and intervention will be a win-win for us all, especially the patients.”